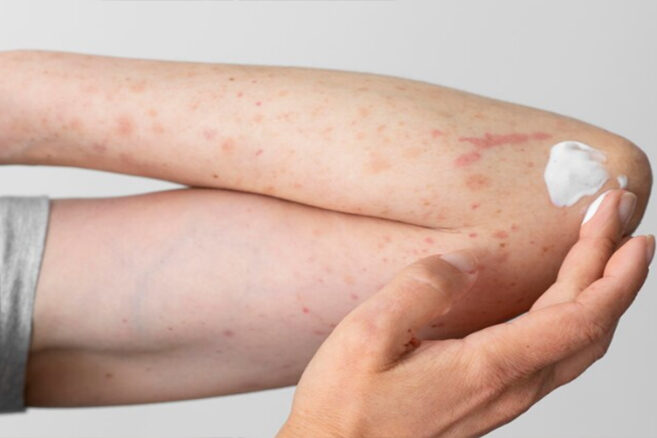
Allergic contact dermatitis is a type of skin inflammation that occurs as a result of contact with a substance to which the body has an allergic reaction. When contact occurs with this substance (allergen), an inflammatory reaction develops on the skin, which leads to various symptoms.
Allergic contact dermatitis can be caused by various substances such as metals (for example nickel), plants (for example poison ivy, poison oak), cosmetic products, medications, dyes, solvents, and many others.
Symptoms of allergic contact dermatitis
Symptoms of allergic contact dermatitis may develop at the site of contact with the allergen and include:
- itching, burning, tingling at the site of contact with the allergen
- redness and inflammation of the skin at the site of contact is one of the early signs of allergic contact dermatitis
- the skin becomes swollen and puffy at the site of contact with the allergen
- blisters and rashes: small fluid filled blisters or skin eruptions appear, vesicular (with blister like formations) or papular (raised skin lesions)
- dryness and flaking of the skin at the site of contact, related to inflammation and disruption of the skin’s natural barrier
- cracks and ulcers with prolonged and intense skin inflammation
Symptoms of allergic contact dermatitis may develop within several hours or days after contact with the allergen.
Diagnosis of allergic contact dermatitis
Diagnosis of allergic contact dermatitis usually includes the following steps:
- medical history: the doctor will conduct a detailed interview to learn about your medical history, including symptoms, factors related to contact with potential allergens, and previous skin reactions
- physical examination: the doctor carefully examines the affected skin to identify signs of allergic contact dermatitis such as redness, swelling, blisters, rash, and other skin changes
- allergen testing at the Medical Expert Complex with doctor consultation:
food, household, contact, pollen, chemical, and drug allergens, assessment of food intolerance, and personalized diet selection - patch tests are the most common method for diagnosing allergic contact dermatitis. Patch tests are performed to determine allergic reactions to specific substances. Small amounts of potential allergens are applied to special patches that are placed on your skin for several days. The doctor evaluates the skin reaction to determine which allergens are causing the reaction.
- exclusion of other possible causes of skin inflammation such as infections, other forms of dermatitis, or autoimmune diseases before establishing the diagnosis of allergic contact dermatitis
Identifying the allergen that causes the allergic reaction is an important step in diagnosing allergic contact dermatitis.
Causes of allergic contact dermatitis
Allergic contact dermatitis can be caused by various substances to which the body reacts in an allergic manner. These substances are called allergens and may have different origins.
Some common causes of allergic contact dermatitis include:
- metals: nickel found in jewelry, jeans buttons, metal fasteners, and other items can cause allergic skin reactions
- plants such as poison ivy, poison oak, and others contain substances that can cause allergic contact dermatitis in sensitive individuals
- cosmetics and perfumes: ingredients such as preservatives, fragrances, and dyes can cause allergic skin reactions
- medications including topical creams, ointments, and patches can cause allergic skin reactions
- chemical substances: solvents, dyes, industrial chemicals, and other chemical agents can cause allergic contact dermatitis
- food products such as nuts, seafood, fruits, and others can cause skin allergic reactions upon contact
- toxin buildup in the body, presence of parasitic infections, and helminth infestations
Parasitic infections can cause allergic dermatitis
Parasites are one possible cause of contact dermatitis, but this is relatively rare. Some parasites may cause irritation, inflammation, and skin reactions in certain people upon contact.
- mites such as spider mites or other types can cause contact dermatitis, leading to redness, itching, and inflammation at the site of contact or bite
- lice: bites from head, body, or pubic lice cause severe itching, irritation, and skin inflammation
- fleas: flea bites can cause skin irritation and allergic reactions in some individuals, especially those sensitive to flea saliva
- Trombicula mites, known as harvest mites, cause intense itching, inflammation, and rash upon contact
Helminth infestations cause allergic dermatitis
Worms such as pinworms (Enterobius vermicularis) and roundworms (Ascaris lumbricoides) do not usually cause allergic contact dermatitis directly. However, they are associated with allergic reactions and symptoms that include skin changes.
When helminths infect the body, they cause various symptoms including itching, inflammation, and skin irritation. One possible mechanism of skin symptoms is an immunological reaction to the presence of worms. In response to infection, the body produces antibodies and other inflammatory mediators, leading to skin irritation and inflammation.
Types of helminth infestations
- nematodes (roundworms)
- roundworms (Ascaris lumbricoides) live in the intestines and may cause itching, hives, and sometimes skin rashes due to allergic reactions to their metabolic products
- pinworms (Enterobius vermicularis) cause severe itching in the anal area, especially at night, and may provoke irritation and dermatitis
- Trichinella (Trichinella spiralis) enters the body through undercooked meat and causes swelling, rash, itching, and muscle pain
- cestodes (tapeworms)
- pork and beef tapeworms (Taenia solium, Taenia saginata) usually do not cause strong skin allergic reactions, but some people may experience itching and hives
- Echinococcus species affect the liver and lungs, and cyst rupture may cause severe allergic reactions including rash and swelling
- trematodes (flukes)
- Schistosoma species affect blood vessels of the bladder and intestines and may cause itchy skin eruptions upon penetration of the skin
Mechanism of skin symptoms in helminth infections
- worms and their metabolic products stimulate production of IgE antibodies
- the immune system responds with inflammation, which may manifest as itching, skin redness, hives, worsening of allergic dermatitis or eczema
Features in children and adults
- in children, skin symptoms are more pronounced due to higher immune sensitivity
- in adults, symptoms may be milder and sometimes limited to occasional itching and rashes
Treatment of allergic contact dermatitis
Treatment of allergic contact dermatitis usually includes several approaches aimed at relieving symptoms and preventing further contact with the allergen. Common treatment methods include:
- Avoid contact with the allergen: the first step is identifying and avoiding the substance that causes the reaction, including changing skincare products, cosmetics, household chemicals, or other items you use
- Use of topical medications: a doctor may recommend anti itching creams, ointments, or lotions to reduce itching, inflammation, and skin irritation
- Skin hygiene: regular moisturizing and proper skin hygiene reduce dryness, flaking, and improve the skin’s natural barrier. Avoid harsh soaps and strong detergents that may irritate the skin
- Anti inflammatory medications: in cases of severe inflammation, a doctor may recommend nonsteroidal anti inflammatory creams or oral medications to reduce inflammation and itching
- Antihistamine medications: a doctor may recommend antihistamines to reduce itching and allergic reactions
- Intravenous ozone therapy: intravenous administration of ozonated saline solution and major autohemotherapy. This method helps quickly and effectively oxygenate the body, improve microcirculation, reduce inflammation, and stimulate immunity. In allergic dermatitis, intravenous ozone therapy helps reduce itching, redness, and swelling, and helps prevent flare ups.
- Administration of ozonated saline solution involves intravenous infusion of sodium chloride solution enriched with an ozone oxygen mixture. The ozonated solution has antibacterial, anti inflammatory, and immunomodulatory effects. For patients with allergic dermatitis, this approach reduces allergic activity, accelerates skin regeneration, and decreases rash and itching.
- Major autohemotherapy for atopic contact dermatitis involves collecting the patient’s blood, treating it with an ozone oxygen mixture, and returning it to the bloodstream. This stimulates the immune system, improves metabolism, and activates protective mechanisms. It helps reduce inflammation, allergic reactions, and supports skin recovery.
- Ozonated olive oil enriched with ozonides is produced by treating olive oil with an ozone oxygen mixture, forming active compounds. It is used for various skin conditions including allergic contact dermatitis and has anti inflammatory, antimicrobial, and wound healing properties.
- Body cleansing program for 5 to 10 days in inpatient or outpatient settings
- accommodation in a single or double room
- examination: doctor consultations, ultrasound of abdominal organs (liver, gallbladder, bile ducts, pancreas, spleen) and kidneys, ECG, testing for viruses, bacteria, parasites, vitamin and microelement deficiencies, food intolerance testing, laboratory tests
- hypoallergenic diet: vegetarian, raw food, juice therapy
- therapeutic fasting for 10 to 15 days
- detox program: cleansing of the intestines, liver, gallbladder, kidneys, antiparasitic and choleretic herbal teas, massage
- ozone therapy methods: intravenous ozonated saline, major autohemotherapy, ENT ozone sanitation, rectal ozone insufflation, ozonated water intake, ozonated oil intake, topical ozonated oil use, vaginal ozone insufflation, periarticular injections of ozone oxygen mixture, urethral and bladder sanitation
- correction of pathological processes using the Medical Expert Complex: targeting parasitic, fungal, and viral flora
- visceral therapy: internal organ massage
- photon therapy
- pressotherapy: mechanical lymphatic drainage massage
- duodenal gallbladder probing
Diet for allergic contact dermatitis
Allergic contact dermatitis is usually caused by contact with allergens applied to the skin. However, there is also another type called atopic dermatitis or eczema, which may be linked to food allergies or intolerances. In atopic dermatitis, diet plays a role in symptom management.
- Consult a doctor: seek medical advice from a doctor or allergist for proper evaluation. The doctor may recommend allergy testing or an elimination diet to identify food triggers
- Food intolerance identification in allergic contact dermatitis using the Medical Expert Complex(MEC) is based on analysis of the dynamic electrical field of the body. The system operates in a passive and safe mode, scanning functional states of organs and regulatory processes to identify individual reactions to foods. The obtained spectral dynamic markers are compared with reference data, allowing the doctor to identify foods that increase allergic inflammation, adjust the diet, and reduce the overall allergic load. The method is non invasive, suitable for adults and children, and is used as part of a comprehensive doctor MEC patient approach for personalized diagnostics and therapy.
- Identify and eliminate food allergens: if food allergens are identified as the cause, an elimination diet is recommended, removing foods such as eggs, dairy, wheat, soy, nuts, fish, and others depending on individual reactions
- Gradual food reintroduction: after elimination, foods are gradually reintroduced to assess the body’s reaction and identify specific triggers
- Maintain a balanced diet: even with restrictions, it is important to maintain balanced nutrition. A doctor can help create a suitable meal plan