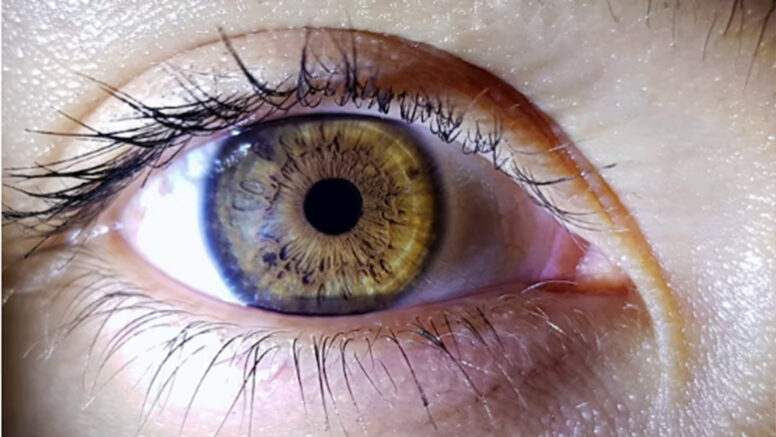
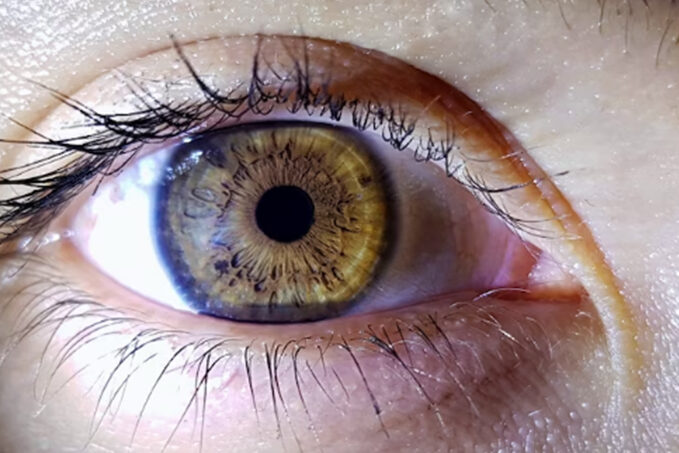
Allergic keratitis is an inflammatory disease of the cornea caused by an allergic reaction. The cornea is the transparent front part of the eye that plays an important role in focusing light onto the retina.
Allergic keratitis can be triggered by various allergens such as plant pollen, animal fur, dust, mold, or contact lenses. When exposed to an allergen, the eye’s immune system responds by releasing certain substances such as histamine, which leads to inflammation and irritation of the cornea.
Symptoms of allergic keratitis:
- Itching and redness of the eyes
- Eye discharge
- Sensation of sand or a foreign body in the eye
- Blurred vision
- Sensitivity to light
Treatment of allergic keratitis may include the use of topical medications such as eye drops with antihistamine or anti-inflammatory effects. In some cases, oral medications may be prescribed. It is also important to avoid contact with known allergens, which can help reduce symptoms.
Causes of allergic keratitis
Allergic keratitis can be caused by an immune system reaction to various allergens. Some of the most common causes include:
Plant pollen: Pollen from various plants such as trees, grasses, and flowers can be a strong allergen. When pollen enters the eyes, the immune system may respond by releasing inflammatory substances, causing keratitis.
Animals: Animals, especially their fur, saliva, and skin flakes, can trigger allergic reactions in some people. If an allergic person comes into contact with animals and then rubs their eyes, this may lead to allergic keratitis.
Dust and dirt: Household dust, mold, and other environmental allergens can cause allergic eye reactions, including keratitis.
Contact lenses: Some people may develop an allergic reaction to the materials used in contact lenses or their cleaning solutions. This may lead to allergic keratitis when wearing contact lenses.
Other factors: Some people may have a genetic predisposition to allergic reactions or atopic conditions such as atopic dermatitis or asthma, which can increase the risk of developing allergic keratitis.
Worms, fungi, viruses, parasites influence the development of allergic keratitis.
The causes of allergic keratitis can vary from person to person, and some individuals may be sensitive to multiple allergens at the same time.
How worms, fungi, viruses, and parasites affect the development of allergic keratitis
Worms, fungi, viruses, and parasites can cause various types of infections in the body, including eye infections, which in turn may lead to the development of allergic keratitis. However, their influence on allergic keratitis is often indirect, through activation of the immune system.
When the body encounters an infection, the immune system becomes activated to fight the infectious agent. During this process, various inflammatory mediators such as histamine, cytokines, and other substances may be released, which can trigger an allergic reaction. This may lead to allergic keratitis in some individuals.
Some specific examples of infections associated with allergic keratitis:
- Viral conjunctivitis: Eye infections caused by viruses such as herpes or herpes simplex virus (HSV) may be associated with the development of allergic keratitis. Viruses can activate the immune system and trigger an allergic response in the cornea.
- Fungal infections: Rare cases of fungal eye infections, such as keratitis caused by Candida or Aspergillus, may sometimes be accompanied by allergic reactions, which can include allergic keratitis.
- Parasitic infections: Some parasitic infections, such as pinworms (Enterobius vermicularis), which affect the intestines, may cause eye irritation and allergic reactions, including keratitis.
The influence of worms, fungi, viruses, and parasites on the development of allergic keratitis is considered one of the contributing factors.
Another important factor in the development of allergic keratitis is the body’s allergic reaction to allergens such as pollen, animals, and other environmental substances.
Treatment of allergic keratitis
Treatment of allergic keratitis is aimed at reducing inflammation and relieving symptoms associated with the condition. Some treatment methods include:
- Avoiding allergens: The first step is identifying and avoiding allergens that trigger the reaction. This may include avoiding plant pollen, contact with animals, using hypoallergenic products, and improving environmental hygiene.
- Topical medications: Eye drops with antihistamine and anti-inflammatory effects may be prescribed to relieve symptoms such as itching, redness, and inflammation. These may include antihistamine drops, mast cell stabilizers, or anti-inflammatory drops.
- Oral medications: In some cases, especially in severe or chronic allergic keratitis, a doctor may prescribe oral antihistamines or anti-inflammatory drugs to enhance the effect and reduce inflammation.
- Treatment of associated conditions: If allergic keratitis is linked to other allergic diseases such as atopic dermatitis or allergic rhinitis, comprehensive treatment may be required to control all symptoms and reduce overall allergic burden.
- Preventive measures: It is important to follow preventive steps to avoid recurrence. This may include wearing sunglasses, regular hand washing, cleaning the environment from allergens, and following medical advice.
- Body cleansing program: An outpatient or inpatient detoxification program lasting 5–10 days. It helps eliminate toxins and waste from the body, restore metabolism, support weight reduction, and improve the function of the intestines, liver, gallbladder, lymphatic, and circulatory systems.
- Antiparasitic therapy
- Ozone therapy methods
- Pressotherapy – аппаратный лимфодренажный массаж for cleansing the lymphatic system
- Visceral massage – massage of internal organs: helps normalize metabolism, reduce intestinal spasms, remove mucus and parasites, reduce visceral fat, and stimulate liver, gallbladder, and pelvic organ function
- Ozone therapy: intravenous administration, rectal insufflation, upper respiratory tract sanitation with oxygen-ozone mixture, intake of ozonated water, ozonated oil
Each case of allergic keratitis is unique, and treatment should be individualized. It is recommended to consult an ophthalmologist for proper diagnosis and an optimal treatment plan.
Types of ozone therapy for inflammatory diseases of the cornea
Ozone therapy is a treatment method based on the use of ozone, an active form of oxygen, aimed at stimulating the immune system and improving metabolic processes in tissues.
Inflammatory diseases of the cornea may be one of the indications for ozone therapy.
Methods of ozone therapy for inflammatory diseases of the cornea:
- Autohemotherapy with oxygen-ozone mixture: A small amount of the patient’s blood is taken, mixed with ozone, and then reintroduced into the body. This may strengthen the immune system and reduce inflammation.
- Intravenous infusion of ozonated saline solution
- Rectal insufflation of oxygen-ozone mixture
- Intake of ozonated water
Hardware lymphatic drainage massage for allergic inflammation of the cornea
Hardware lymphatic drainage massage (pressotherapy) is a supportive treatment method for allergic inflammatory diseases of the cornea.
It is used to improve lymphatic circulation and reduce swelling, helping to decrease inflammation and associated symptoms.
This method involves the use of special devices that create gentle vacuum pressure on the body, stimulating the lymphatic system, improving fluid drainage, and removing toxins from tissues. As a result, swelling and inflammatory symptoms around the eye are reduced.
A comprehensive approach to treating allergic inflammation of the cornea may be the most effective for achieving positive results.
Body cleansing course in the treatment of allergic inflammation of the cornea
- To determine the cause of the disease and factors influencing chronic or acute conditions, an additional comprehensive body analysis on the Medical Expert Complex is performed.
Assessment of all organs and systems includes: immune system status; allergens; viral load; bacterial load; fungal load; detected helminths; vitamin and micronutrient deficiencies; ENT organs; bronchopulmonary system; cardiovascular system; gastrointestinal tract; liver and gallbladder; pancreas; kidneys and bladder; reproductive organs; musculoskeletal system; nervous system; endocrine system; and unsuitable food products.
After determining the causes of the disease, the medical center “Alternative” provides a full-body recovery program based on the author’s method of the chief physician Olga Vladimirovna Timchenko.
- Outpatient or inpatient detox program lasting 5–10 days. It helps remove toxins, restore metabolism, reduce weight, and improve the function of the intestines, liver, gallbladder, lymphatic, and circulatory systems.
Examinations: abdominal ultrasound, laboratory tests, and body analysis using the Medical Expert Complex.
Detox program: accommodation; nutrition; herbal teas; massages; ozonated water; rectal insufflation with oxygen-ozone mixture; ear canal insufflation; cleansing enemas; blind probing of the gallbladder and liver (tubage); cleansing of the small and large intestines.
Why cleanse the liver when treating allergic inflammation of the cornea?
Liver function may be an important factor in the treatment of allergic inflammation of the cornea.
Treatment may include various medications such as antihistamines, anti-inflammatory drugs, and eye drops.
The liver plays a key role in the processing and metabolism of many medications, including those used for treating allergic inflammation. It filters and breaks down these drugs, ensuring safe absorption and preventing toxic buildup.
If liver function is impaired due to disease or certain medications, it may affect drug metabolism, potentially increasing side effects or reducing treatment effectiveness.
Why gallbladder cleansing is necessary in the treatment of allergic inflammation of the cornea
The gallbladder has no direct role in treating allergic inflammation of the cornea. It stores and releases bile needed for fat digestion and does not directly affect allergic processes.
However, some people with allergies may have associated conditions such as food allergies or allergic rhinitis. In rare cases, severe allergic reactions may cause discomfort in the gallbladder area.
If you have gallbladder conditions such as gallstones or chronic cholecystitis, medical consultation is necessary to adjust treatment. Some medications may affect gallbladder function, which is why supportive cleansing procedures are sometimes considered.
In any case, personalized medical advice from a doctor is essential.
Connection between gastrointestinal diseases and allergic inflammation of the cornea
There is a connection between gastrointestinal diseases and allergic inflammation of the cornea. Studies and clinical observations suggest that disorders of the gastrointestinal tract may contribute to allergic reactions, including eye inflammation.
One possible explanation is the “gut–eye axis.” Changes in the gut microbiome and increased intestinal permeability may trigger inflammatory responses and immune activation affecting not only the gut but also other organs, including the eyes.
Some gastrointestinal diseases such as irritable bowel syndrome (IBS), Crohn’s disease, ulcerative colitis, and celiac disease may be associated with a higher risk of allergic reactions and eye inflammation. However, further research is needed to fully understand these mechanisms.
Treatment of gastrointestinal diseases associated with allergic reactions may include detoxification programs, dietary correction, restoration of the gut microbiome, and immune system support.